Trigeminal Neuralgia
What You Need to Know
Trigeminal neuralgia is a chronic pain condition that causes sudden, sharp, electric shock-like facial pain. Recognizing trigeminal neuralgia symptoms early can lead to quicker diagnosis and more effective treatment. It originates from the trigeminal nerve, which carries sensation from your face to your brain. At Red Butte Pain Solutions, we specialize in diagnosing and treating trigeminal neuralgia, helping patients across Arizona reclaim their lives. It is considered one of the most painful conditions in medicine and can greatly interfere with daily life.
Recognizing Trigeminal Neuralgia Symptoms and Triggers
Trigeminal neuralgia symptoms often begin subtly and grow more severe over time. The hallmark symptom is brief but intense facial pain that may feel like a lightning strike. This pain usually affects one side of the face and can last from a few seconds to a couple of minutes.
Common Symptoms Include
-
-
Sudden, stabbing, or shock-like facial pain
-
Pain triggered by light touch, chewing, talking, or brushing teeth
-
Pain in the jaw, cheek, lips, gums, or around the eye or ear
-
Pain episodes that occur in rapid succession or in clusters
-
A burning or tingling sensation between attacks
-
Sensitivity to wind, cold, or vibration on the face
-
These symptoms often follow a recognizable pattern and can become more intense and frequent with time. As attacks worsen, they may interfere with eating, speaking, brushing teeth, or simply being outdoors on a windy day. This growing intensity can severely impact day-to-day comfort, social interactions, and emotional well-being.
Common Triggers
-
-
Brushing your teeth
-
Talking or smiling
-
Eating or chewing
-
Washing your face
-
Shaving or applying makeup
-
Cold air or wind blowing across the face
-
Recognizing and understanding these triggers can help patients manage their symptoms and avoid unnecessary pain flares. By identifying patterns and avoiding known stimuli, patients may be able to reduce the frequency and intensity of trigeminal neuralgia episodes. This proactive approach plays a key role in improving daily comfort and minimizing disruption to everyday life.
Causes of Trigeminal Neuralgia
Trigeminal neuralgia occurs when the trigeminal nerve, which transmits sensation from the face to the brain, becomes irritated or compressed. This nerve is unique because it transmits pain signals directly to the brain without passing through any signal-relay points, or “switches,” along the way. This direct connection may explain why pain from trigeminal neuralgia feels so sudden and severe. Several underlying conditions can contribute to this disruption.
Common Causes
-
-
Vascular compression: A blood vessel can loop around or press against the trigeminal nerve at its root entry zone near the brainstem. This constant pulsating pressure may wear away the protective myelin sheath that insulates the nerve, leading to erratic, overactive pain signals. Vascular compression is one of the most common causes of classic trigeminal neuralgia and is often identified through advanced imaging techniques like MRI.
-
Multiple sclerosis (MS): This chronic neurological disease disrupts communication between the brain and the body by damaging the protective sheath (myelin) that insulates nerves. When MS affects the trigeminal nerve, it can result in severe facial pain resembling classic trigeminal neuralgia. This pain may be more persistent and less responsive to traditional treatments, making MS-related trigeminal neuralgia a distinct clinical challenge.
-
Tumors: A growth such as a benign or malignant tumor can press on the trigeminal nerve, disrupting its normal function and triggering episodes of intense facial pain. While tumors are a less common cause of trigeminal neuralgia, it is important to identify them early through imaging. In some cases, tumor-related nerve compression may also be associated with other neurological symptoms such as numbness, vision changes, or balance problems.
-
Injury or trauma: Facial or dental surgeries, including root canals or wisdom tooth removal, may inadvertently irritate or damage the trigeminal nerve. Even minor procedures or facial injuries can lead to inflammation or scarring near the nerve, resulting in chronic pain. In some cases, blunt trauma from an accident or fall may trigger symptoms of trigeminal neuralgia weeks or months later.
-
Aging: Natural aging processes can affect the structure and function of nerves, making them more vulnerable to dysfunction. As we age, the protective myelin sheath that surrounds nerves may deteriorate, increasing the risk of misfiring pain signals. Additionally, age-related changes in blood vessels or bone structure may lead to compression or irritation of the trigeminal nerve.
-
Shingles: Reactivation of the varicella-zoster virus can cause a painful skin rash and nerve inflammation, particularly when it affects the facial region. This inflammation can directly involve the trigeminal nerve, resulting in severe, stabbing pain. In some cases, even after the shingles rash has healed, patients may experience lingering nerve pain known as post-herpetic neuralgia (PHN), which can mimic or worsen trigeminal neuralgia symptoms. Early treatment of shingles may reduce the risk of long-term nerve pain.
-
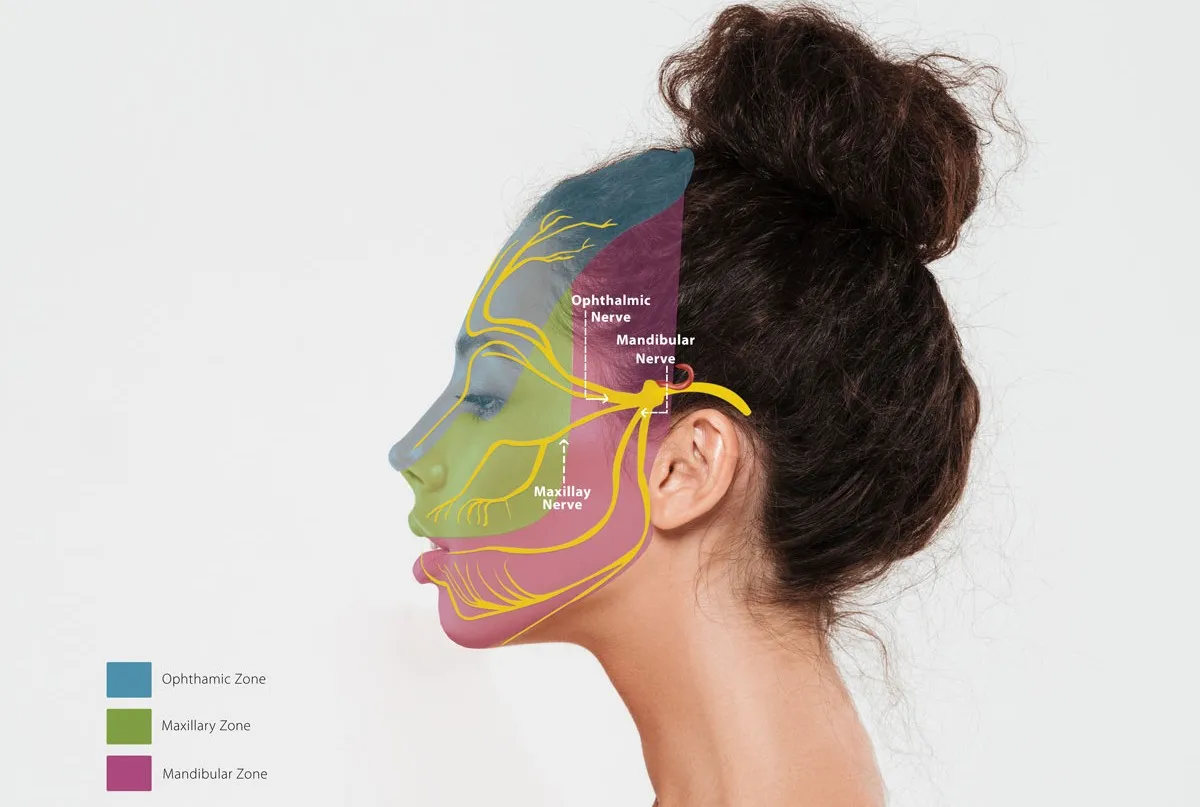
Diagnosing Trigeminal Neuralgia
Diagnosing trigeminal neuralgia starts with a detailed medical history and physical examination. Your healthcare provider will evaluate your symptoms and rule out other potential causes of facial pain.
Diagnostic Tools May Include
-
-
Neurological exam: This exam evaluates how well your facial nerves respond to different types of stimulation. Your provider may test your reflexes, muscle strength, and facial sensation using light touch or pinprick tools to determine if your pain pattern is consistent with trigeminal neuralgia.
-
MRI or CT scans: These imaging tools help detect underlying causes such as tumors, multiple sclerosis, or vascular compression. MRI is especially useful for viewing the brain and trigeminal nerve path. CT scans help rule out structural abnormalities in the skull or facial bones.
-
Blood tests: Blood work helps rule out infections, autoimmune diseases, or other systemic conditions that might mimic or worsen facial pain. While not used to diagnose trigeminal neuralgia directly, these tests are useful in building a complete clinical picture.
-
Accurate diagnosis ensures you receive the most effective treatment for your specific condition.
Treatment Options for Trigeminal Neuralgia
Related Topics:
Trigeminal neuralgia can be managed through a combination of medications, interventional procedures, and surgery. Treatment plans depend on the severity of symptoms and how well initial therapies work.
Medications
-
-
Anticonvulsants: Such as carbamazepine and oxcarbazepine to stabilize nerve activity
-
Muscle relaxants: Like baclofen to reduce nerve-related spasms
-
Interventional Treatments
-
-
Trigeminal nerve blocks: Injections that deliver numbing medication directly to the nerve to reduce pain
-
Trigeminal nerve ablation: A procedure that disrupts pain signals by targeting specific branches of the trigeminal nerve
-
Surgical Options
-
-
Microvascular decompression (MVD): A neurosurgical procedure that relieves pressure from a compressing blood vessel
-
Rhizotomy: A procedure that selectively destroys nerve fibers to stop pain signals
-
Treatment usually begins with medication. If medications are ineffective or cause significant side effects, procedures like nerve blocks, ablation, or surgery may be considered. Each treatment plan is customized to the patient’s needs to ensure safe and effective care.
Trigeminal Neuralgia and Neuropathic Pain
Trigeminal neuralgia is a form of neuropathic pain, which results from damage or dysfunction in the nervous system. Unlike other pain types caused by tissue injury or inflammation, neuropathic pain arises from misfiring or damaged nerves.
Patients with trigeminal neuralgia often describe their pain as sharp, burning, or electric. These symptoms are common in many neuropathic pain conditions. Therefore, treatment strategies such as nerve blocks, medications, and neuromodulation techniques often overlap across different neuropathic conditions.
Relief Is Within Reach
Living with trigeminal neuralgia can feel overwhelming, but you don’t have to suffer alone. At Red Butte Pain Solutions, we understand how debilitating facial nerve pain can be. Our compassionate team is here to help you find lasting relief.
We proudly serve patients in Chandler, Ahwatukee, Tempe, Phoenix, Gilbert, Mesa, Sun Lakes, Maricopa, Casa Grande, and Laveen, Arizona.
📞 Call us today at 602-633-4334
📅 Or Schedule now to begin your personalized care journey.
Understanding Facial Pain and Trigeminal Neuralgia
Facial pain can be one of the most distressing and intense types of pain a person can experience. In 2020, I faced this firsthand when a tooth infection spread into my face, causing unbearable pain. The infection led to emergency surgery, and even with just a 50%...
