Painful Diabetic Neuropathy
How Common Is Diabetic Neuropathy?
Diabetic neuropathy is a common complication of diabetes mellitus, characterized by nerve damage resulting from prolonged high blood sugar levels. This condition primarily affects the peripheral nerves, and as a result, it can lead to symptoms ranging from mild discomfort to severe pain and disability.
Diabetic neuropathy affects approximately 50% of people with diabetes during their lifetime. Among individuals with type 2 diabetes, about one in four may already have neuropathy at diagnosis. Painful diabetic neuropathy specifically impacts 20% to 30% of those with diabetic peripheral neuropathy. This condition is not only common but also, more importantly, one of the most disruptive forms of nerve pain caused by diabetes. Individuals with painful diabetic neuropathy often experience daily challenges that affect their sleep, mood, and mobility.
Pathology of Diabetic Neuropathy
Having high blood sugar for a long time can damage your nerves. This happens because extra sugar in your blood changes the way your body works. Sticky sugar particles can build up and, over time, get in the way of how nerves send signals. At the same time, high blood sugar can hurt the tiny blood vessels that bring oxygen and nutrients to your nerves. Without enough oxygen and nutrients, your nerves can slowly become weak and eventually stop working the right way.
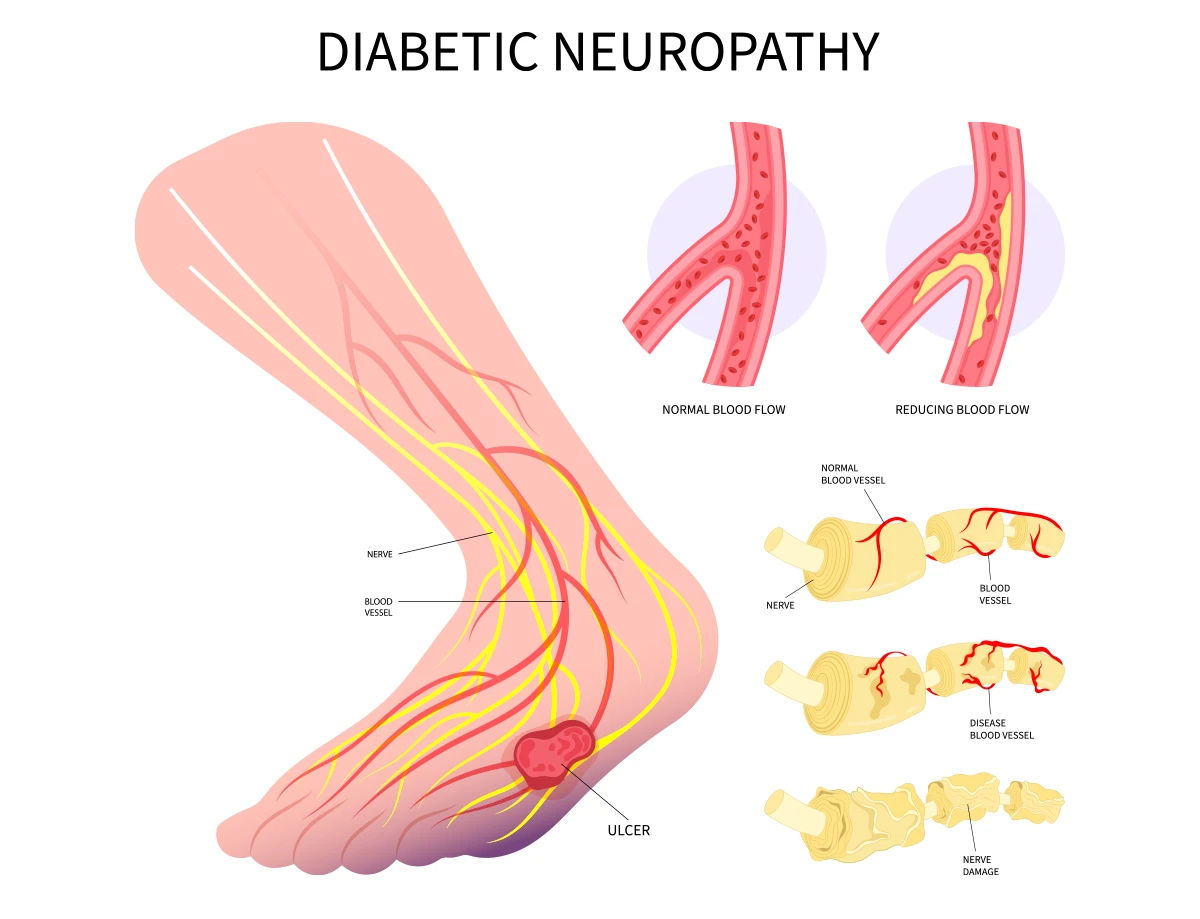
Symptoms of Diabetic Neuropathy
Symptoms vary depending on the type of nerves affected:
Sensory Neuropathy
The most common form, it affects nerves that transmit sensations. Symptoms include:
-
-
Tingling and numbness: A pins-and-needles sensation, often in the feet or hands, that may spread upward.
-
Loss of ability to feel pain: Minor injuries may go unnoticed, increasing the risk of infections.
-
Loss of temperature sensitivity: Inability to detect hot or cold surfaces can lead to burns or frostbite.
-
Loss of coordination: Diminished feedback from the feet impairs balance and walking.
-
Burning or shooting pain: Often worse at night, these sharp pains can disrupt sleep and daily life.
-
Motor Neuropathy
This involves nerves that control muscle movement. Symptoms include:
-
-
Muscle weakness: Muscle shrinkage may develop, making movement more difficult.
-
Loss of reflexes: Decreased leg and foot responsiveness can affect stability.
-
Difficulty with motor tasks: Actions like buttoning shirts or walking may become challenging.
-
Autonomic Neuropathy
This affects involuntary functions and can cause:
-
-
Digestive issues: Gastroparesis may cause nausea, bloating, and erratic blood sugar.
-
Urinary problems: Difficulty emptying the bladder or incontinence.
-
Sexual dysfunction: Erectile dysfunction in men, and decreased arousal in women.
-
Blood pressure instability: A drop in blood pressure upon standing can cause dizziness.
-
Risks Associated with Diabetic Peripheral Neuropathy
Diabetic peripheral neuropathy (DPN) carries serious health risks:
-
-
Foot ulcers and infections: Injuries often go unnoticed and can develop into ulcers. Untreated ulcers may become infected and require amputation.
-
Amputation and its consequences: Diabetes is the leading cause of non-traumatic lower-limb amputations. Among those with below-the-knee amputations, nearly 50% will not survive more than five years. For above-the-knee amputations, over 70% of patients die within five years—rates higher than many cancers.
-
Balance and coordination issues: Nerve damage increases fall risk.
-
Chronic pain: Painful diabetic neuropathy can reduce quality of life and contribute to sleep problems, depression, and anxiety.
-
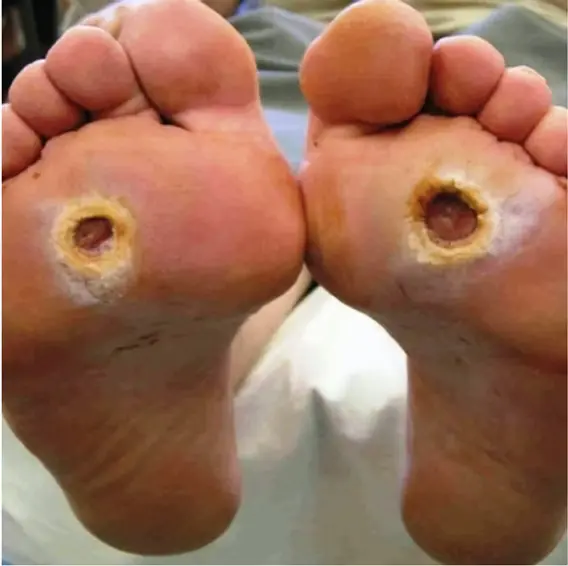
Treatment of Painful Diabetic Neuropathy
Treating painful diabetic neuropathy involves several strategies. Specifically, these are aimed at relieving symptoms and, more importantly, improving daily function and comfort:
Medications
Painful diabetic neuropathy can be difficult to treat, but several medication options are available to manage the pain. According to the National Institute for Health and Care Excellence (NICE), and supported by emerging clinical research:
-
-
Antidepressants: Certain antidepressants, such as amitriptyline and duloxetine, are commonly used to treat painful diabetic neuropathy. These medications not only help relieve pain but can also improve sleep and mood, which are often affected by chronic nerve pain. They work by changing the levels of chemicals in the brain and spinal cord that are involved in sending pain signals. While they are not the same as antidepressants used for depression, they can still be very effective for nerve-related pain when taken as prescribed.
-
Anticonvulsants: Gabapentin and pregabalin are frequently used to relieve symptoms of painful diabetic neuropathy. These medicines were originally designed to prevent seizures, but they also work well for calming overactive nerves. They help stop the nerves from sending too many pain signals to the brain. People who use these drugs often report less burning, tingling, and shooting pain in their feet and legs. It may take time to feel the full effects, and some people may feel sleepy or dizzy when starting these medications.
-
Topical treatments: Capsaicin cream may reduce localized pain by targeting certain pain receptors in the skin. It is made from chili peppers and causes a warm or burning sensation when first applied, but over time it can help lessen the skin’s ability to register pain. This option is most effective when used regularly and applied to specific painful areas, like the feet in painful diabetic neuropathy.
-
Ketamine infusions: Low-dose ketamine, given through an IV, may help reduce nerve pain in some patients who haven’t responded to other treatments. It works by blocking NMDA receptors that help transmit pain signals.
-
Lidocaine infusions: Lidocaine given through an IV can calm irritated nerves and reduce pain. Some studies show that lidocaine infusions may be helpful for people with painful diabetic neuropathy when oral medications aren’t enough.
-
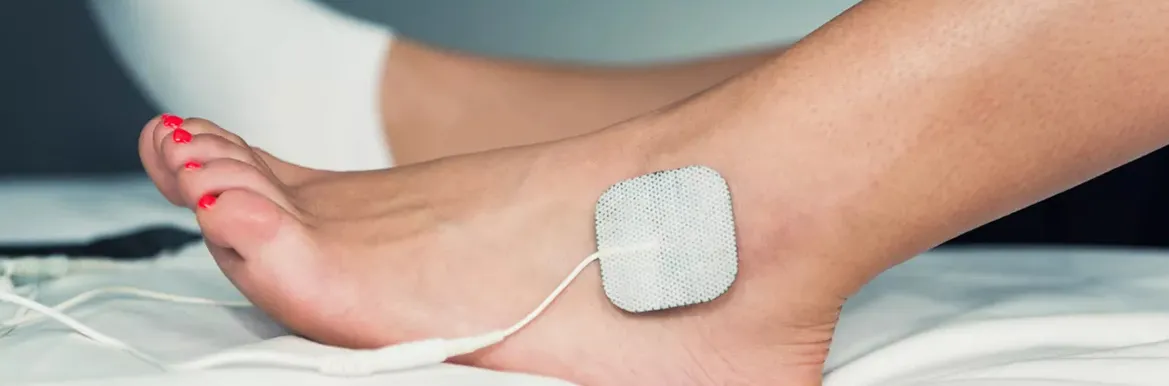
Physical Therapy
For those with painful diabetic neuropathy, physical therapy offers drug-free support that complements other treatments. Engaging in physical therapy can help maintain strength and function:
-
-
Exercise programs: Improve blood flow and support nerve healing.
-
Manual therapy: Relieves deep pain, cramping, and muscle tightness.
-
Balance training: Reduces fall risk through improved coordination.
-
Lifestyle Modifications
Simple changes can slow progression and relieve symptoms of painful diabetic neuropathy:
-
-
Blood sugar control: Crucial for slowing nerve damage.
-
Healthy diet: Supports overall nerve function.
-
Regular exercise: Boosts circulation and improves energy.
-
Quit smoking: Enhances blood flow and promotes healing.
-
Advanced Treatment Options
Some people with painful diabetic neuropathy do not find relief through medication or therapy alone. For resistant cases, advanced therapies include:
-
-
Spinal Cord Stimulation (SCS): A device is implanted near the spinal cord to block pain signals. Studies show that high-frequency (10-kHz) SCS provides significant relief. In a clinical trial with 216 patients, 79% receiving 10-kHz SCS reported major pain reduction compared to just 5% in the control group.
-
Transcutaneous Electrical Nerve Stimulation (TENS): A non-invasive option using low-voltage electrical currents for temporary relief. Often available for home use.
-
Take Control of Your Pain
If you’re living with painful diabetic neuropathy, know that help is available and relief is possible.
Early detection and treatment of painful diabetic neuropathy are key to avoiding complications. A multidisciplinary plan combining medication, physical therapy, and lifestyle changes can help you regain comfort and function. To take the next step in managing your symptoms, call 602-633-4334 to schedule an appointment with Red Butte Pain Solutions today.
Is Diabetic Nerve Pain Reversible?
"Is diabetic nerve pain reversible?" This is one of the most common questions I hear from patients at Red Butte Pain Solutions. Diabetic peripheral neuropathy (DPN) can be frustrating and life-changing, especially when patients feel like their symptoms are progressing...
Is Heel Pain a Sign of Cancer? Rare but Important to Know
Heel pain is one of the most common foot complaints, affecting people of all ages and activity levels. For most individuals, it results from everyday wear and tear, overuse, or minor injuries related to walking, running, or standing for long periods. Conditions like...
Nerve Pain in Cancer: Causes and Relief Options
Nerve pain in cancer—also known as neuropathic cancer pain (NCP)—is a complex and often debilitating type of pain. It affects a significant number of patients either due to direct tumor invasion or as a side effect of cancer treatments like surgery, chemotherapy, or...
What Are the Risk Factors for Painful Diabetic Neuropathy?
Understand what increases your chances of developing nerve pain from diabetes—and how to prevent it. Living with diabetes already requires constant attention to your health. But for many people, the real trouble starts when painful diabetic neuropathy sets in. This...
Do Stims Stim? 20-Years of Spinal Cord Stimulation Innovation
Over the last 20 years, spinal cord stimulation has transformed significantly. It’s evolved from a basic pain relief option to a sophisticated, adaptable therapy with specialized features. When spinal cord stimulators (SCS) first emerged, they offered hope but little...
Do Stims Stim? The HFX Spinal Cord Stimulator
Introduction At Red Butte Pain Solutions, we’re always exploring new options for effective pain relief, including spinal cord stimulator (SCS) devices. Many of you may have read our recent post on Differential Targeted Multiplex (DTM) stimulation, where we covered its...
Breaking New Ground in Pain Management: DTM and Closed-Loop Spinal Cord Stimulation
When I was in training, I was taught that "Stims stim," meaning there wasn’t much difference between spinal cord stimulation (SCS) devices beyond customer service for our patients. Back then, no SCS devices had MRI compatibility, and the only real debate was whether...
Fighting Diabetic Neuropathy: A Personal Journey
Diabetic Neuropathy: A Pathway to Loss About 12 years ago, I lost my cousin, well, technically my mother's cousin, to complications from diabetes. He was a funny, gregarious, larger-than-life individual who always made me laugh, gave sage advice, and was fun to be...
Understanding and Treating Diabetic Peripheral Neuropathy at Red Butte Pain Solutions
Living with diabetic peripheral neuropathy, often referred to as diabetic nerve pain, can be incredibly challenging. At Red Butte Pain Solutions, located in Chandler, Arizona, we understand the unique struggles faced by those in our community dealing with this...