Trigeminal Nerve Ablation
Radiofrequency Ablation of the Trigeminal Nerve
Exploring Trigeminal Neuralgia and the Role of Ablation
Trigeminal neuralgia is a severe facial pain condition that affects daily life and emotional well-being. Patients describe it as a sharp, electric shock-like pain that affects the cheek, jaw, or around the eye. The pain can be sudden, intense, and debilitating. For many, daily activities like brushing teeth, eating, or even feeling a breeze on the skin can trigger unbearable pain. When medications no longer control these symptoms, radiofrequency ablation of the trigeminal nerve may provide lasting relief. At Red Butte Pain Solutions, we specialize in fluoroscopically guided trigeminal nerve ablation—a minimally invasive procedure targeting the nerve at the foramen ovale to treat trigeminal neuralgia effectively and safely.
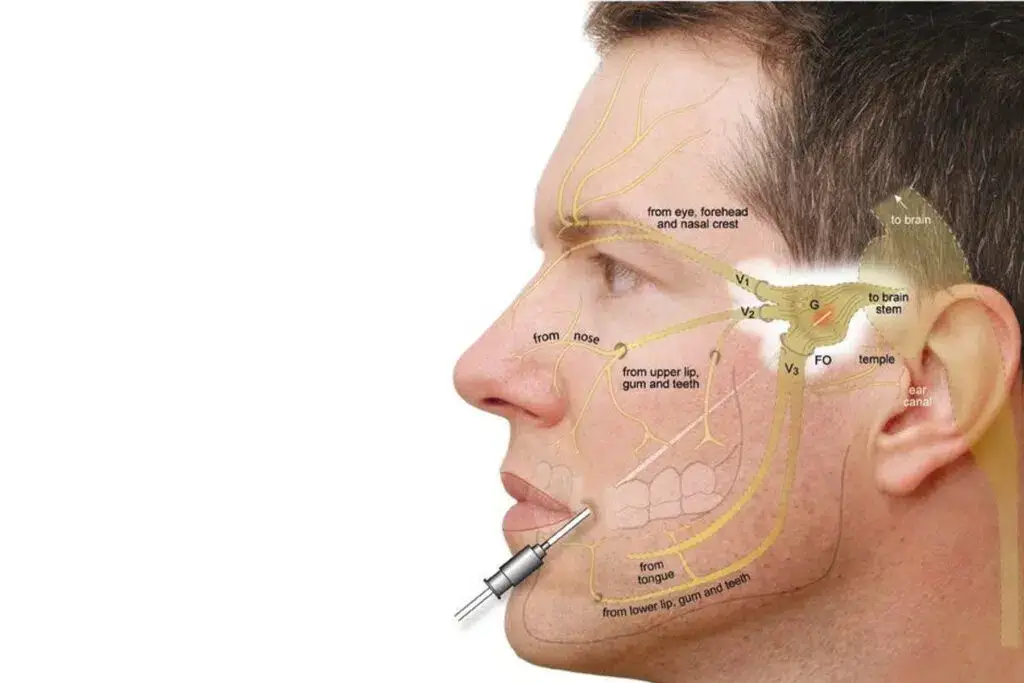
How Trigeminal Nerve Ablation Works
Radiofrequency ablation of the trigeminal nerve uses controlled heat to disrupt pain signals at their source. The procedure targets the trigeminal ganglion, a cluster of nerve cells where sensory signals from the face enter the brain. By applying heat through a specialized needle, a small lesion is created on the nerve, interrupting the transmission of pain while preserving other functions.
This treatment differs from surgical decompression or gamma knife radiosurgery because it avoids cutting or irradiating tissues. Instead, it offers a repeatable, outpatient procedure with immediate feedback on accuracy using electrical stimulation. Fluoroscopy allows the physician to visualize the bony landmarks, especially the foramen ovale, ensuring safe and accurate needle placement.
What Is the Foramen Ovale?
The foramen ovale is a small, oval-shaped hole in the base of the skull. It serves as an exit point for the mandibular branch (V3) of the trigeminal nerve. During fluoroscopically guided radiofrequency ablation, a thin, specialized needle is passed through the patient’s cheek to reach this location.
Using real-time X-ray imaging (fluoroscopy), the needle is guided safely to the target. Once it enters the foramen ovale, the physician confirms placement with motor and sensory stimulation. Only after confirming the correct nerve branch is involved does the ablation begin. This method minimizes the risk of damaging adjacent nerves or tissues.
Who Is a Candidate for Trigeminal Nerve Ablation?
Candidates for trigeminal nerve ablation often have classical trigeminal neuralgia with pain affecting one side of the face, usually the lower face or jaw. The pain may respond initially to medications like carbamazepine or oxcarbazepine, but over time, many patients find that the relief diminishes or the side effects become intolerable.
This procedure is especially effective for patients with conditions such as:
-
- Face pain limited to one or two branches of the trigeminal nerve
- Multiple sclerosis-related trigeminal nerve pain
- Postherpetic neuralgia (shingles pain) involving the trigeminal nerve
It is also useful for patients who are not candidates for open neurosurgery due to age or medical conditions. Because it is repeatable and does not burn bridges for future treatments, trigeminal nerve ablation offers a valuable middle ground between medication and invasive surgery.
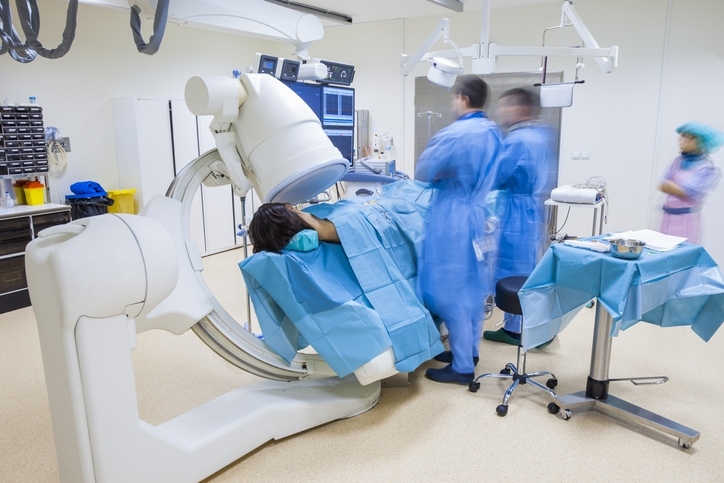
What to Expect Before, During, and After the Procedure
Before the procedure, patients undergo a comprehensive evaluation. This includes a detailed history, neurological exam, and imaging studies such as MRI to rule out other causes of facial pain. Patients may be asked to temporarily stop certain medications, especially blood thinners, before the procedure. Fasting is usually required for at least six hours prior.
On the day of the procedure, patients arrive at an outpatient surgical center or medical office. They will first meet with an anesthesiologist to discuss their health history, review the sedation plan, and confirm that they have followed the required NPO (nothing by mouth) instructions. After this, light sedation is given, and the patient is positioned on their back with the head slightly extended. The cheek is cleaned and numbed.
A thin radiofrequency needle is inserted through the cheek and advanced toward the foramen ovale under fluoroscopic guidance. Once the needle is in position, the physician performs sensory and motor testing to ensure the correct branch of the trigeminal nerve is targeted. After testing, the nerve is treated with controlled heat for 90 seconds. The entire procedure usually takes under 30 minutes.
Recovery begins immediately after. Patients are monitored for a short time, then discharged with post-procedure instructions. Facial numbness or tingling may be noticed immediately. Some patients feel soreness in the cheek or jaw, but this typically resolves within days.
Benefits of Trigeminal Nerve Ablation
Trigeminal nerve ablation is favored for its minimally invasive nature and strong track record of success. There are no incisions, stitches, or lengthy hospital stays. It is performed entirely on an outpatient basis. Most importantly, the procedure allows patients to avoid long-term reliance on pain medications, which often have side effects such as drowsiness, dizziness, or liver toxicity.
Patients commonly report rapid relief from facial pain, better sleep, and improved mood. Many return to normal daily activities within a day or two. This level of functional improvement makes trigeminal nerve ablation a life-changing intervention for those living with constant, severe facial pain.
Potential Risks and Side Effects
Like all medical interventions, trigeminal nerve ablation carries some risks. The most common side effect is numbness in the area of the face treated. While this may feel strange, most patients prefer it to the sharp, lancinating pain of trigeminal neuralgia. In rare cases, the numbness can be bothersome or permanent.
There is a small risk of jaw weakness, especially when the mandibular nerve is targeted. Corneal numbness is a rare but serious complication if the ophthalmic branch (V1) is affected, as it can lead to eye injuries. This is why careful testing and imaging are essential. Other rare risks include bleeding, infection, allergic reaction to medications, or anesthetic complications.
Fortunately, when performed by experienced physicians using fluoroscopic guidance, trigeminal nerve ablation is considered safe and well-tolerated. The ability to fine-tune the lesion size and temperature further enhances its safety profile.
Outcomes and Success Rates
Numerous studies and decades of clinical experience support the effectiveness of radiofrequency ablation of the trigeminal nerve at the foramen ovale. Between 80% and 90% of patients experience immediate pain relief following the procedure. One-year pain-free rates range between 60% and 70%. Repeat procedures may be performed if pain recurs, often restoring relief without diminishing success rates.
In some patients, the pain returns gradually as the nerve regenerates. The procedure can be repeated with similar success. Unlike destructive surgeries that cut the nerve permanently, radiofrequency ablation allows targeted treatment with minimal disruption to overall nerve function.
Patients with multiple sclerosis or postherpetic neuralgia may have lower response rates, but even partial relief can be meaningful for quality of life. Overall, trigeminal nerve ablation remains a cornerstone in the treatment of chronic facial pain.
Recovery and Follow-Up Care
After the procedure, most patients go home the same day. Some choose to take the day off from work, while others resume light activity within 24 hours. Facial numbness or tingling is common and often lasts several weeks. This sensation is usually not painful and tends to fade gradually.
Patients should avoid rubbing or scratching the numb area to prevent injury. If the eye is involved, lubricating drops or protective eyewear may be recommended. A follow-up visit is scheduled within 1–2 weeks to assess the results and monitor for any recurrence of pain. Close follow-up helps ensure optimal outcomes and allows adjustments to future care if needed.
Why Choose Red Butte Pain Solutions?
At Red Butte Pain Solutions, our board-certified physicians are highly trained in advanced image-guided pain procedures. We take pride in offering personalized care using the safest and most effective techniques available. Fluoroscopically guided trigeminal nerve ablation is one of our areas of expertise, and we have helped countless patients reclaim their lives from the grip of facial pain.
We work closely with neurologists, primary care providers, and neurosurgeons to ensure you receive comprehensive, coordinated care. From consultation to recovery, our team supports you every step of the way.
Take the Next Step Toward Relief
If you suffer from facial pain that hasn’t responded to medications, trigeminal nerve ablation may offer lasting relief. Don’t let facial pain define your life. Call Red Butte Pain Solutions today at 602-633-4334 or Schedule now to explore your options and take the next step toward a life with less pain.
Understanding Facial Pain and Trigeminal Neuralgia
Facial pain can be one of the most distressing and intense types of pain a person can experience. In 2020, I faced this firsthand when a tooth infection spread into my face, causing unbearable pain. The infection led to emergency surgery, and even with just a 50%...
