Experiencing persistent nerve pain after inguinal hernia surgery can be both unexpected and distressing.
While hernia repairs are among the most common surgeries, some patients develop chronic postoperative pain, especially from nerve involvement. This article explores the causes of nerve pain, compares surgical techniques, and outlines the most effective treatment options for long-term relief.
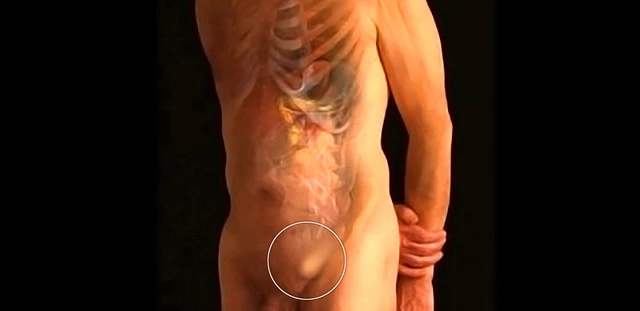
Nerve Pain After Inguinal Surgery
Chronic pain after inguinal hernia repair, also known as post-herniorrhaphy neuralgia, affects 10–12% of patients. Some studies report even higher rates. This pain often results from nerve damage or irritation sustained during the surgical procedure.
Nerves Involved in Hernia Surgery
Several nerves in the groin can be affected during hernia repair. The ilioinguinal nerve provides sensation to the upper inner thigh and genital region. The iliohypogastric nerve supplies the lower abdomen and upper outer thigh. The genitofemoral nerve has two branches—one supplying the scrotum or labia majora, and the other serving the upper thigh. Damage or entrapment of any of these nerves can lead to long-term, burning, or shooting pain.
Causes of Nerve Pain After Hernia Surgery
There are many potential causes of nerve pain after hernia surgery. Surgical trauma may occur if nerves are cut, stretched, or caught in sutures. The surgical mesh used in repairs can irritate or compress nearby nerves. Neuromas—painful nerve growths—can form at the site of nerve injury. Additionally, scar tissue can entrap nerves, causing persistent pain.
Comparing Hernia Surgery Techniques
Open hernia repair involves a larger incision and direct access to the hernia site. Although effective, this method carries a higher risk of nerve injury due to increased tissue manipulation and may result in more postoperative pain.
Laparoscopic hernia repair uses smaller incisions and a camera to guide the surgeon. This technique generally results in less pain after surgery but still carries some risk of nerve damage, especially when performed by less experienced surgeons.
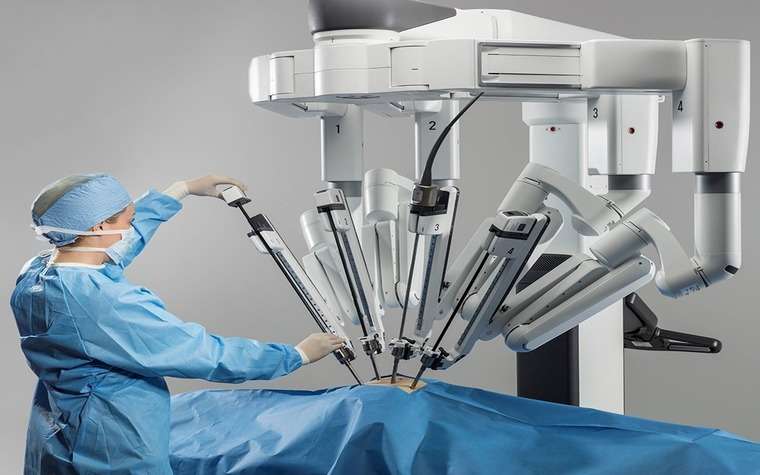
Robotic-assisted hernia repair enhances the laparoscopic method by offering greater precision and visualization. While it may lower the risk of complications, long-term data on nerve injury outcomes is still being gathered.
Regardless of the technique, surgeon skill and experience are critical in minimizing the risk of nerve pain after inguinal surgery.
Treatment Options for Nerve Pain
First-line treatments often include medications that help calm irritated nerves. Gabapentin and pregabalin are commonly used to manage neuropathic pain. Antidepressants such as amitriptyline and duloxetine may also be beneficial by altering how the brain processes pain. Topical medications like lidocaine and capsaicin can provide local relief.
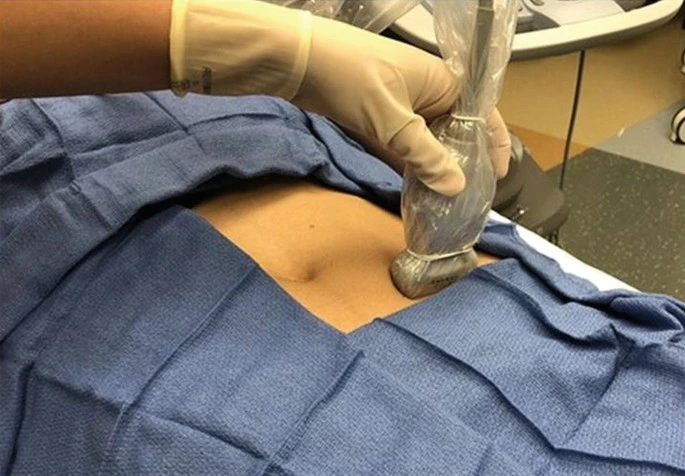
Ultrasound-guided nerve blocks offer both diagnostic and therapeutic benefits. These injections deliver anesthetic and steroid medication directly to the affected nerve, offering temporary relief and helping to confirm the source of pain. Repeat injections may be needed in some cases.
Surgical neurectomy, or removal of the damaged nerve, is an option when other treatments fail. While this can provide significant pain relief, it often results in permanent numbness in the affected area and is typically considered a last resort.
Radiofrequency ablation (RFA) is a minimally invasive technique that uses heat to interrupt pain signals in the targeted nerve. It can provide long-term relief for patients with chronic inguinal neuralgia and is performed with imaging guidance.
Peripheral Nerve Stimulation
Peripheral nerve stimulation (PNS) is an innovative treatment for patients whose pain persists despite conservative care. This technique involves placing a small electrical lead near the affected nerve to deliver gentle impulses that interfere with pain signals before they reach the brain. The procedure is minimally invasive and guided by imaging.
For individuals with ilioinguinal or genitofemoral neuralgia, PNS can significantly reduce pain and improve daily function. The system is adjustable and reversible, offering a non-destructive, flexible option for long-term pain management. At Red Butte Pain Solutions, we carefully assess patients for PNS after they have exhausted simpler treatments.
Lidocaine and Ketamine Infusions
Lidocaine infusions can block pain signals at the spinal level and are sometimes used to treat neuropathic pain like post-herniorrhaphy neuralgia. A 2014 review in Anesthesia & Analgesia found that lidocaine may offer relief for post-surgical nerve pain, although more research is needed.
Ketamine infusions represent another option for patients with severe or resistant pain. Ketamine acts by blocking NMDA receptors involved in chronic pain processing. Although effective for some, ketamine can cause side effects such as hallucinations and changes in heart rate. A 2013 article in Pain Physician supports its use in carefully selected patients.
Both therapies are considered when traditional methods fail and are administered under strict monitoring at Red Butte Pain Solutions.
Patient Outlook and Recovery Expectations
Not every patient with nerve pain after hernia surgery will have lifelong symptoms. Many experience steady improvement with medications, physical therapy, and interventions like nerve blocks or RFA. Having a customized care plan and early involvement of a pain specialist can enhance recovery.
It’s important to recognize that nerve pain recovery is not always linear. Symptoms may fluctuate, especially during periods of stress or increased physical activity. Monitoring pain levels, response to treatments, and overall function helps tailor ongoing care. Collaboration between surgeons and pain specialists is vital, especially if symptoms last longer than three to six months.
Strategies for Prevention
Preventing chronic nerve pain begins in the operating room. Surgeons should identify and protect critical nerves during the procedure. Choosing the right type and size of mesh, and placing it with precision, helps avoid nerve contact. Educating patients on symptoms of nerve pain and encouraging prompt reporting also supports early diagnosis and treatment.
Get Relief from Hernia-Related Nerve Pain
Chronic nerve pain after hernia surgery can be life-altering—but effective treatments are available. At Red Butte Pain Solutions, we offer a comprehensive approach that includes nerve blocks, medications, radiofrequency ablation, lidocaine infusions, and neuropathic pain therapies. We also offer cutting-edge options like peripheral nerve stimulation.
Call us today at 602-633-4334 or Schedule now to begin your journey toward pain relief.
